How Perimenopause Changes Your Brain
And why thinking feels so completely, disorienting different
Edited & Reviewed by Kira Hensley, M.A., M.Ed., Registered Psychotherapist ~ Women's Mental Health, Anxiety & Perimenopause
Updated March 2026. 7 min read
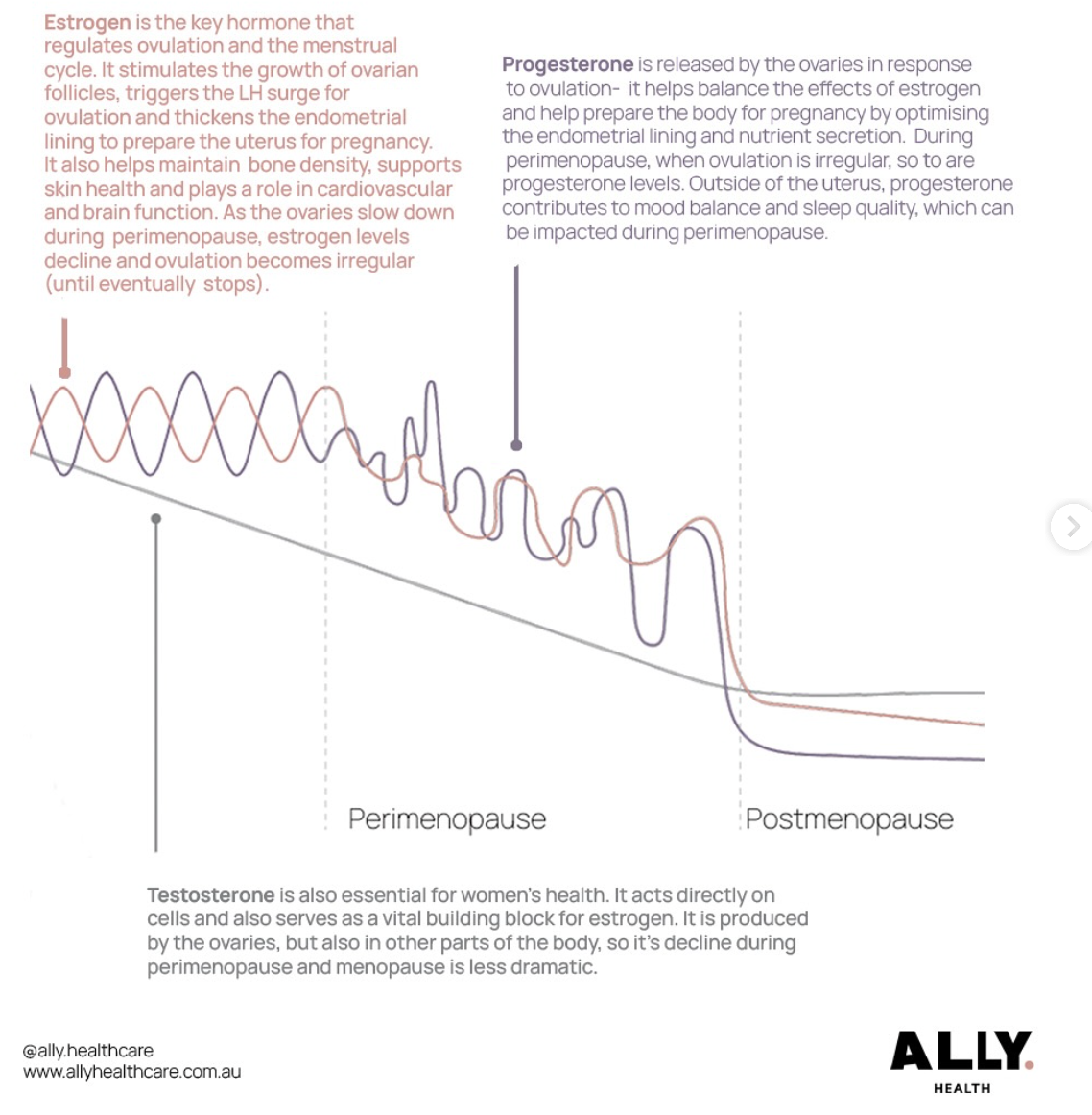
Perimenopause brings a new hormonal environment for the female brain.
Key Takeaways:
Perimenopause brain changes — including brain fog, memory lapses, word-finding difficulties, and impaired concentration — are real, neurologically documented, and not a sign that something is permanently wrong with you.
These changes result from a layered interaction between fluctuating estrogen (which directly affects brain function), disrupted sleep, and the compounding cognitive demands of midlife stress.
For most women, the most significant cognitive symptoms cluster during the perimenopausal transition itself and improve as the brain adapts — and there are evidence-informed strategies that help in the meantime.
You walk into a room and forget why you came. You lose a word mid-sentence that you've used thousands of times. You reread the same paragraph four times and still can't hold it. Your concentration, once reliable, now fractures at the slightest interruption — and the mental agility you built over decades seems to have quietly packed its bags.
If this sounds familiar, you are not losing your mind. You are in perimenopause — and perimenopause brain changes are among the most common, least discussed, and most distressing aspects of this transition. The fact that most women are never told they're coming makes them even harder to bear.
This post is here to change that. Below, you'll find a section-by-section breakdown of what's actually happening in your brain, why it feels the way it does, and what a genuinely helpful path forward looks like — one that acknowledges biology, sleep, stress, and the full weight of midlife, not just hormones in isolation.
What Is Actually Happening to Your Brain During Perimenopause?
You're not imagining it
So many women arrive in therapy convinced something is seriously wrong — that they are developing early dementia, or that they have simply "lost" the sharp, capable person they used to be. If that fear has crossed your mind, you are in enormous company. The cognitive changes of perimenopause are among the most under-discussed and most genuinely frightening symptoms of this transition, precisely because no one prepared you for them.
What the neuroscience tells us
Estrogen is not just a reproductive hormones — it plays a critical role in brain health. It supports the production of acetylcholine and serotonin, protects neurons from inflammation, and regulates blood flow to key cognitive regions. During perimenopause, estrogen doesn't simply decline in a straight line; it fluctuates erratically, and the brain — calibrated to its rhythms for decades — has to work harder to compensate for each unpredictable shift.
This biological disruption rarely operates in isolation. Midlife often brings compounding stressors — caregiving for ageing parents, career pressures, children, relationship changes — and chronic stress elevates cortisol, which directly impairs hippocampal function and working memory. Sleep disruption, another hallmark of perimenopause, compounds everything further: a sleep-deprived brain is a cognitively impaired brain, regardless of hormone levels. This is what we call the “biopsychosocial picture” — there’s not one cause, but a layered convergence of several factors.
A path forward
Begin by naming what's happening as a neurological transition, not a personal failing. Keeping a simple symptom journal — noting sleep quality, stress level, and cognitive difficulties together — can help you and your healthcare providers see the full picture, rather than addressing each symptom in isolation.
📖 Further reading: North American Menopause Society (NAMS) — Menopause and the Brain
Why Does Perimenopause Cause Brain Fog and Mental Fatigue?
You're not imagining it
That feeling of trying to think through wet concrete — where even simple tasks feel effortful and your thoughts seem to drift before you can catch them — is one of the most commonly reported and least validated symptoms of perimenopause. You are not lazy, and you are not being dramatic. Brain fog and mental fatigue during this transition are physiologically real, and they have a clear neurological explanation.
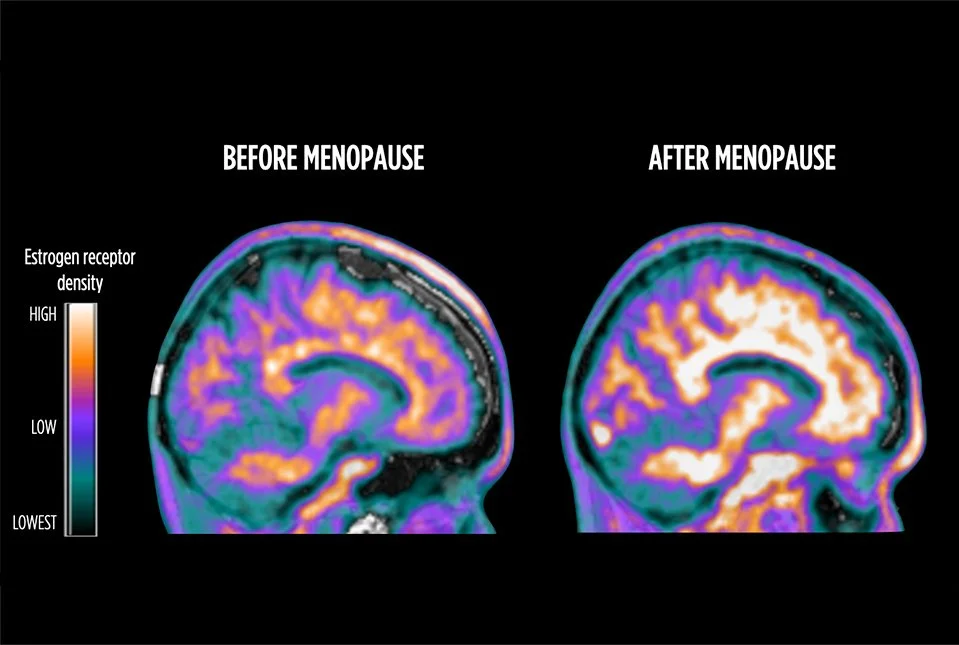
Estrogen receptor density increases in the brain during the transition, possibly to accommodate the declining estrogen available. From Mosoni, L. et al. 2024. In vivo brain estrogen receptor density by neuroendocrine aging and relationships with cognition and symptomatology, Scientific Reports, 14, 12680.
What the neuroscience tells us
Estrogen influences mitochondrial function in brain cells, which means fluctuating levels can reduce the energy available for cognitive processing — literally making thinking harder at a cellular level. At the same time, estrogen withdrawal disrupts the brain's default mode network, the system responsible for background integration and that sense of mental fluency we usually take for granted.
When sleep is disrupted by night sweats or hyperarousal, the brain's glymphatic system — which clears metabolic waste during deep sleep — cannot do its job properly, leaving a build-up of neural debris that directly contributes to that foggy, sluggish feeling the next day. Chronic stress adds another layer: sustained high cortisol reduces glucose uptake in the prefrontal cortex, the region most responsible for clear, organised thought. This is a biopsychosocial cascade, not a character flaw.
A path forward
Prioritising sleep — even imperfect, interrupted sleep — is one of the highest-leverage interventions available. Strategic rest during the day, even 10–15 minutes of quiet, screen-free downtime, can partially restore cognitive clarity without requiring a full nap or a complete schedule restructure.
Why Is Your Memory Struggling During Perimenopause?
You're not imagining it
Forgetting the name of your favourite pasta dish, re-reading the same paragraph four times, walking to the car and having no recall of the route — these moments can feel genuinely frightening, especially if you've watched a parent navigate cognitive decline. It's important to say clearly: perimenopause-related memory changes are different from dementia, and for the vast majority of women, they are temporary.
What the neuroscience tells us
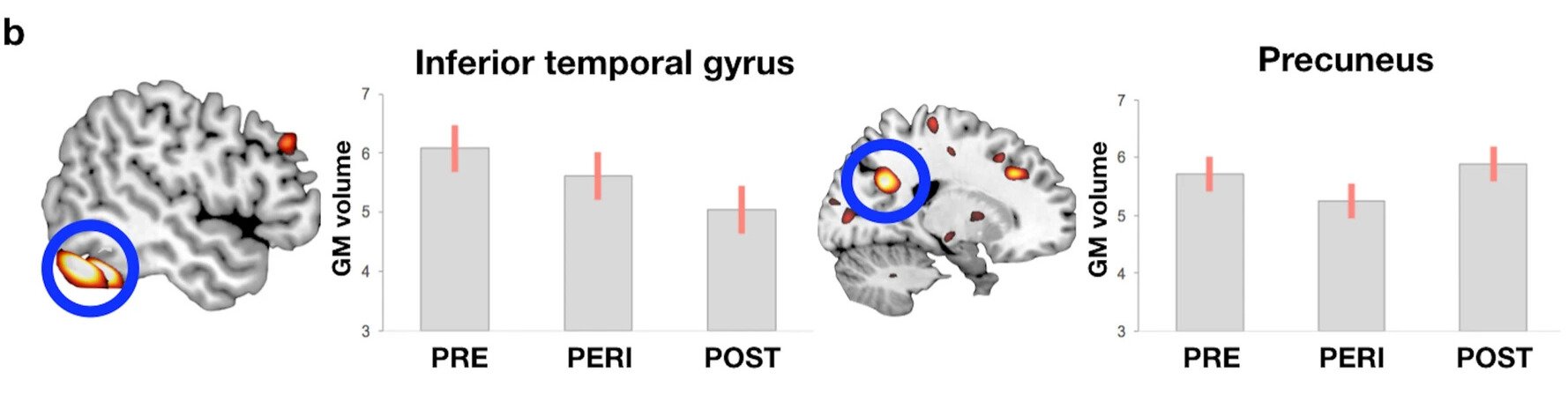
The hippocampus — the brain's primary memory consolidation centre — is densely packed with estrogen receptors, making it particularly sensitive to hormonal fluctuation. Verbal memory and episodic memory (the memory of events and experiences) tend to be most affected, while procedural memory — how to do things — typically remains intact. Research consistently shows that memory difficulties tend to peak during the perimenopause transition itself, then stabilise or improve in postmenopause as the brain adapts.
Sleep is inseparable from memory consolidation: the hippocampus encodes new memories during slow-wave sleep, so disrupted sleep doesn't just leave you tired — it literally interrupts the filing process. The cognitive demands of midlife — the mental load, the emotional labour, the sheer number of things being tracked simultaneously — further crowd out the attentional resources that memory formation requires.
A path forward
External memory systems — visible calendars, voice memos, written lists — are not signs of weakness; they are wise neurological adaptations for a transitional period. Give yourself permission to write things down without framing it as evidence of decline.
📖 Further reading: Maki & Henderson (2016) — Cognition and the Menopause Transition (NIH/PubMed)
Why Can't You Concentrate or Multitask the Way You Used To?
You're not imagining it
If you've noticed that you can no longer hold three things in your head at once, that a single interruption completely derails your train of thought, or that you now need far more silence and protected time to get anything done — this is not a productivity failure. Many women describe this shift as one of the most destabilizing aspects of perimenopause, particularly those in demanding careers or who carry heavy caregiving loads at home.
Multi-tasking?! How did I do this before?
What the neuroscience tells us
Sustained attention and multitasking are primarily functions of the prefrontal cortex, which is exquisitely sensitive to estrogen. As estrogen fluctuates, dopamine and norepinephrine signalling in this region becomes less consistent, reducing the brain's ability to filter distractions and hold multiple streams of information simultaneously.
What we call "multitasking" is actually rapid task-switching, managed by the prefrontal cortex — and this becomes significantly more effortful when neurochemical support is unreliable. The ambient anxiety that often accompanies perimenopause — worrying about symptoms, hormonal mood shifts, life changes — consumes working memory resources that would otherwise be available for focus. Sleep deprivation narrows attentional bandwidth further. The brain is not broken; it is overwhelmed.
A path forward
Single-tasking is not a luxury during perimenopause — it is a neurologically-sound strategy. Structured time-blocking, reducing notification load, and openly communicating your need for fewer interruptions at work and home are practical, evidence-aligned responses, not accommodations to be embarrassed by.
Why Do You Lose Words Mid-Sentence During Perimenopause?
You're not imagining it
The thought is fully formed, you know exactly what you want to say — and then the word simply isn't there. You might pause, gesture, say "the thing" or "you know what I mean," and feel a flush of embarrassment or quiet alarm. This tip-of-the-tongue experience becomes noticeably more frequent during perimenopause, and it can feel uniquely humiliating for women who have always been precise and articulate communicators.
What the neuroscience tells us
Word retrieval relies on a network including the left temporal lobe and prefrontal cortex, both of which are estrogen-sensitive. Estrogen supports verbal fluency partly through its effects on cholinergic pathways — the neural circuits involved in language processing, attention, and memory retrieval. When estrogen fluctuates, the retrieval pathway becomes less efficient, particularly under conditions of fatigue, stress, or the time pressure of fast-moving conversation.
Critically, this is a retrieval problem, not a storage problem — the words are still there; the filing system is temporarily less efficient. Anxiety about word-finding can itself worsen it: the threat response narrows the attentional bandwidth needed for smooth language access, creating a frustrating, self-reinforcing loop.
A path forward
Slowing down in conversation — pausing, breathing, giving yourself permission to come back to a word — actually helps neurologically by reducing the cortisol spike that blocks retrieval. You do not need to apologize for pausing; your brain simply needs a moment more than it used to.
How Does Perimenopause Affect Executive Function?
You're not imagining it
Executive function is the brain's CEO — it handles planning, organising, decision-making, emotional regulation, and the ability to start tasks you don't feel like doing. If decisions have started to feel harder than they should, if you're more easily overwhelmed by complexity, or if your emotional responses feel less filtered than usual — these are executive function changes, and they are among the most underreported perimenopause brain changes of all.
What the neuroscience tells us
The prefrontal cortex, which orchestrates executive functions, undergoes measurable changes during perimenopause as oestrogen support decreases. Estrogen modulates the balance of dopamine in this region — the same neurotransmitter governing motivation, initiation, and cognitive flexibility. Reduced dopaminergic tone can make starting difficult or novel tasks feel disproportionately hard, and emotional regulation — itself an executive function — becomes more effortful.
This is compounded by what is often happening in midlife more broadly: many women are simultaneously navigating role transitions, grief, significant identity shifts, and a fundamental reassessment of priorities — all of which require substantial executive resources at precisely the time those resources are stretched thin. Sleep deprivation impairs the prefrontal cortex more severely than almost any other brain region, creating a particularly relentless feedback loop.
A path forward
Break large tasks into the smallest possible next steps — this reduces the initiation burden on an already-taxed prefrontal cortex. Therapy can be genuinely useful here: working with a therapist to identify which stressors are consuming executive resources — and which can be reduced, delegated, or grieved — creates real neurological head space.
What Actually Helps With Perimenopause Brain Changes?
You're not imagining it
It can feel deeply demoralising to be handed another list of lifestyle recommendations when you are already exhausted, stretched thin, and holding more than any one person should. What you need first is acknowledgement: you are managing something genuinely hard, and the healthcare system is not yet well-equipped to support it fully. The strategies below are evidence-informed options to choose from, not a prescription for perfection.
What the research points toward
Sleep is consistently the highest-leverage intervention — even modest, imperfect improvements in sleep quality produce measurable cognitive gains.
Aerobic exercise increases BDNF (brain-derived neurotrophic factor), which supports neuroplasticity and mood, and specifically protects hippocampal volume over time.
Stress reduction is not optional from a neurological standpoint: chronic high cortisol is directly neurotoxic, particularly to the hippocampus, making mind-body practices like mindfulness, yoga, and therapy protective rather than indulgent.
Reducing cognitive load through external systems and deliberate delegation.
Genuine self-compassion around productivity is itself a form of brain care.
A path forward
Choose one area — sleep, movement, stress, or medical support — and make one specific, sustainable change this week, rather than overhauling everything at once. A perimenopause-informed therapist can help you identify which domain will give you the most relief given your specific situation and history.
📖 Related: How Exhaustion Changes Everything: Perimenopause & Sleep
FAQs About Perimenopause Brain Changes
Is perimenopause brain fog the same as early dementia?
No — and this distinction matters. Perimenopause brain changes are tied to hormonal fluctuation and are typically temporary, improving as the brain adapts to post-menopausal hormone levels. Dementia involves progressive, irreversible neurological damage with a distinctly different pattern of decline — affecting daily functioning in ways that perimenopause brain fog does not. If the fear is persistent and affecting your quality of life, a neuropsychological evaluation can provide concrete clarity and genuine peace of mind. But for most women, what they are experiencing is a hormonal transition, not a neurodegenerative one.
Will my memory and concentration come back after menopause?
For most women, yes. Research consistently shows that the most significant perimenopause brain changes cluster during the transition itself, and many women report noticeable improvement in cognitive clarity once they reach postmenopause and hormone levels stabilize at a new baseline. The trajectory varies between individuals — which is precisely why supporting your brain health now through sleep, exercise, and stress management matters — but the evidence does not support the fear that these changes are permanent for the majority of women.
Why does anxiety feel so much worse during perimenopause — and how is that connected to my thinking?
The connection between worsening anxiety and cognitive difficulties is direct and neurological. Estrogen and progesterone have a regulatory effect on the amygdala — the brain's threat-detection centre. As estrogen fluctuates, the amygdala becomes more reactive and the prefrontal cortex has less capacity to modulate it. This means anxiety doesn't just feel worse during perimenopause; it actively impairs the cognitive functions — concentration, memory, word retrieval — that you're already trying to protect. Treating the anxiety is therefore also treating the cognitive symptoms, and therapy is particularly well-placed to do both simultaneously.
📖 For more on anxiety during perimenopause, read my post distinguishing Perimenopause Anxiety from General Anxiety.
Should I be worried that I can't multitask like I used to at work?
You don't need to be worried — but you do need to adapt, and you deserve support in doing so. Difficulty multitasking efficiently is one of the most practically disruptive perimenopause brain changes for working women, and one of the least accommodated in workplace culture. Rather than pushing through, the evidence supports restructuring how you work: time-blocking, actively reducing interruptions, and communicating your needs clearly. Many women find that addressing sleep, stress, and sometimes hormone levels significantly restores their functional work capacity. If your workplace cannot accommodate reasonable adjustments, that is a structural problem — not a reflection of your capability.
The Bottom Line
Perimenopause brain changes are not a sign that you are losing your mind, falling apart, or failing at midlife. They are the result of a complex, layered neurological transition — one in which fluctuating hormones, disrupted sleep, and the accumulated weight of midlife stress converge in ways that are real, measurable, and, for most women, temporary.
Biology is not the whole story, and the whole story is not a crisis. Understanding what is happening — and why — is itself a form of relief. You are not broken. You are in transition.
The path forward isn't about doing more. It's about understanding your brain well enough to give it what it actually needs right now.
📖 If you want a broader picture of perimenopause and mental health, start with my Definitive Guide on Perimenopause.
If you're navigating perimenopause and would like support that takes both the neuroscience and the emotional weight seriously, I work with women at exactly this intersection. Therapy in perimenopause isn't about coping better or trying harder; it's about understanding yourself more fully. I have in-person sessions in Whitby, ON, and virtual across Ontario.
Related Reading
Perimenopause and Sleep: Menopause, Sleep, and Mood: How Exhaustion Changes Everything
Mood Changes in Perimenopause: Is This Anxiety, Depression, or Hormones?
Midlife Identity Changes: How Perimenopause Affects Your Sense of Self
The information on this website is for informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment or to replace your relationship with your health care provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read or seen on this site.