Perimenopause Rage & Irritability: Why You’re So Angry
Edited & Reviewed by Kira Hensley, M.A., M.Ed., Registered Psychotherapist ~ Women's Mental Health, Anxiety & Perimenopause
Updated March 2026. 5 min read
Key Takeaway: Rage and irritability during perimenopause are real, common, and rarely explained by hormones alone. Fluctuating estrogen lowers your emotional threshold, but burnout, disrupted sleep, and years of swallowed needs are almost always part of the picture too. Understanding the full picture — and working with it intentionally — is what actually changes things.
If you're thinking I'm not an angry person — so why do I feel furious? — I want you to know I hear that question from perimenopausal women in my therapy room more than almost any other.
Maybe it's snapping at your partner for breathing too loudly. Maybe it's an impatience with your kids that feels completely out of character. Maybe you hold it together all day, and then one small thing tips you — and what comes out frightens you.
And then, almost immediately, comes the shame.
Who am I right now? What is wrong with me?
Here is what I want you to hold while you read this: this is almost never a personality change. It's a capacity squeeze — a nervous system with less margin, a life with more load, and sometimes a long-overdue reckoning with what you are no longer willing to carry.
This post will help you understand why it's happening, what it's actually made of, and what — including therapy — genuinely helps.
What does “perimenopause rage” actually look like?
I want to name this carefully, because the way most women describe it to me doesn't match what they expected "rage" to look like — and that mismatch often leads them to dismiss or minimise what they're experiencing for far too long.
For many of my clients, it isn't explosive outbursts. It's a hair-trigger irritability that feels entirely out of character. The noise that suddenly feels unbearable. The interruption that tips you straight into overwhelm. A surge of heat that is wildly disproportionate to the situation in front of you.
A lot of women also describe moving from calm to flooded very quickly, and taking far longer to recover than they used to. Some describe a low-grade grinding edge that never quite settles. Others experience distinct spikes — sharp, fast, followed by disorientation and shame.
It's also common for anger and tears to arrive together, sometimes within the same minute. That combination tends to deepen the shame spiral: I'm not just angry, I'm falling apart.
In therapy, one of the most relieving things I see happen is when a client simply has what she's experiencing accurately reflected back to her. Not labelled as a problem — recognized as a signal. That recognition is where the work begins.
📖 If your irritability is happening alongside a weird emotional flatness, that’s not uncommon—here’s a deeper look at anhedonia in perimenopause.
Why does your emotional threshold drop during perimenopause?
Often, women brace themselves when the hormonal explanation comes up — either they've been dismissed with it before ("it's just hormones") or they're worried it means something is fundamentally wrong with them. Neither is the right frame.
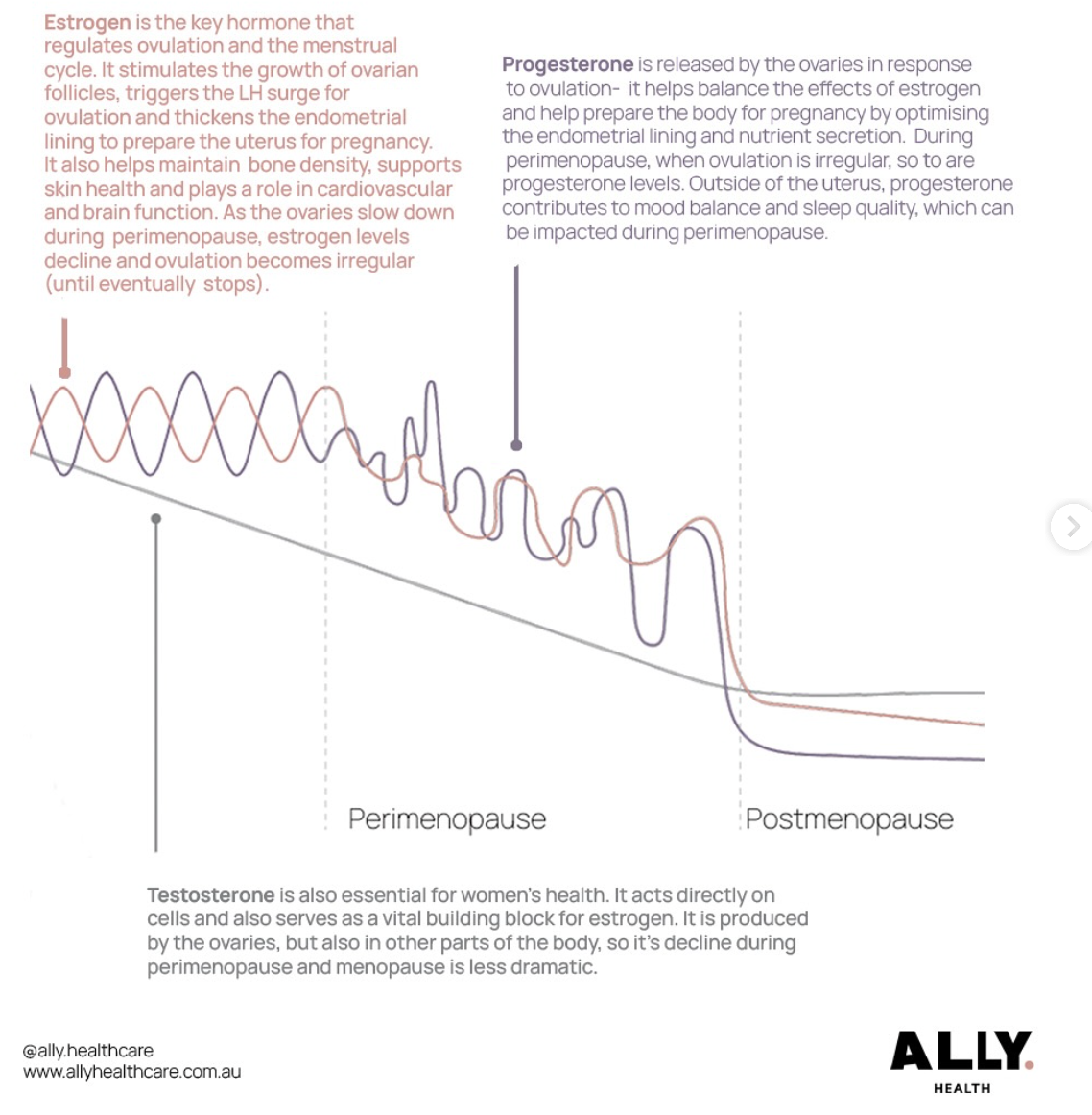
The hormonal piece is real, and it's worth being precise about. Perimenopause isn't usually a smooth decline — it's a period of significant and unpredictable fluctuation. Estrogen and progesterone rise and fall in ways that don't follow the relatively consistent pattern of earlier reproductive years.
Those fluctuations directly affect serotonin and GABA — the neurotransmitters most closely tied to mood regulation and stress response. The practical result is a more sensitized emotional baseline: it takes less to feel overloaded, less to feel flooded, and longer to recover once you do. The North American Menopause Society confirms that mood changes in perimenopause are more closely tied to this variability than to simple hormonal decline.
This is why you might feel emotionally steady one week and completely reactive the next, with nothing obvious changing externally. The landscape has shifted underneath you.
In therapy, I use mindfulness-based approaches to help clients build what's called interoceptive awareness — the ability to notice when your threshold is dropping before you cross it. That early awareness is often the difference between a moment of heat and a blow-up you later regret.
📖 If your irritability is arriving with a constant edge of worry, this may help you sort what’s hormonal and otherwise: perimenopause anxiety vs general anxiety.
What does burnout have to do with how ragey you feel?
This is the piece I find myself returning to most consistently in sessions — because for many women, perimenopause doesn't create the anger so much as it removes the buffer that was keeping it quietly managed.
Midlife is frequently peak demand. Many of my clients are simultaneously parenting teenagers, supporting aging parents, navigating the most intensive years of a career, and carrying the invisible weight of running a household — all while their body is changing in ways they didn't fully anticipate.
Chronic stress has real physiological consequences. It elevates cortisol, disrupts sleep, and steadily narrows the window of tolerance for frustration. Longitudinal research from the SWAN study found that psychosocial stress and life demands contribute significantly to mood symptoms in perimenopausal women, independently of hormonal changes.
When perimenopause adds hormonal variability into an already depleted system, the margin disappears. Anger in this context is often the body's most honest signal: something is asking more from me than I currently have to give.
In ACT-based work, I help clients get clear on the difference between what they're doing because it aligns with their values and what they're doing because they've never stopped to question whether it should be their responsibility at all. That distinction alone can be quietly life-changing.
Why does your body suddenly feel like it has no buffer?
The answer to this is multi-factorial.
Sleep disruption is one of the most consistent experiences of perimenopause, and its effect on emotional regulation is direct. The part of the brain responsible for moderating impulse and softening reactions is particularly vulnerable to fragmented sleep. When sleep is disrupted, the pause between stimulus and response shortens dramatically.
Fuel is a related variable that often gets overlooked. Estrogen plays a direct role in insulin sensitivity and glucose regulation, and as levels fluctuate during perimenopause, blood sugar stability can become genuinely harder to maintain — meaning the sharp, fast-arriving irritability that comes from going too long without eating is a documented physiological response, not a personal failing. The mid-afternoon crash in particular can turn a manageable day into an overwhelming one.
There is also a well-documented increase in sensory sensitivity during perimenopause, linked to the role estrogen plays in modulating the central nervous system's threat-detection response. Noise, clutter, heat, being touched, multiple conversations at once — things previously tolerated without effort can begin to feel like genuine intrusion on an already stretched nervous system. This is not you becoming intolerant. It is your nervous system responding to a real shift in its regulatory environment.
Before interrogating the emotional meaning of a spike, I always ask my clients to check the basics first: sleep, fuel, sensory load. Mindfulness-based work in therapy helps develop the habit of catching these physical states early — before they've already tipped into reactivity.
📖 This is also where a lot of women start doubting themselves—if that’s you, read Why Perimenopause Makes You Feel Like You’re Losing It — and Why You’re Not for a grounding reframe.
Is your anger pointing to something genuinely unfair?
This is the piece that most often gets skipped — including, sometimes, in therapy — and I think it's one of the most important.
There is a cultural script that says anger in perimenopausal women is irrational, out of proportion, something to be managed back into quietness. I want to push back on that directly. Anger is information. And sometimes what it is pointing to is genuinely unjust.
Midlife often brings a particular kind of clarity. Years of invisible emotional labour become harder to unsee. Patterns of inequity in relationships or workplaces become harder to accommodate. The habit of softening your own needs so others stay comfortable becomes exhausting in a way it previously wasn't.
Sometimes perimenopause doesn't create anger. It removes the coping mechanism that was keeping legitimate anger quiet. And the small thing that finally tipped you — the question about the scissors, the request at 9pm — isn't actually about scissors. It's an accounting.
In parts-based therapy, I work with clients to identify which part of them is angry and what it's protecting. That question — what is this anger guarding? — often opens up territory that has been carefully sealed for years. It is some of the most meaningful work I do with clients.
Why does the shame spiral after snapping make things worse?
The moment after a blow-up is often as hard as the blow-up itself. The shame that rushes in feels immediate and total — and it's worth understanding what it does physiologically, because the way most women respond to it actively increases the likelihood of the next spike.
Shame activates the stress response. When you move rapidly into self-criticism after an outburst — I'm a terrible mother, I'm losing control, what is wrong with me — you are adding fuel rather than extinguishing it. The shame response tightens the nervous system and narrows the window of tolerance for the next frustration.
It also obscures what the anger was communicating in the first place. The valid need underneath the sharp delivery gets buried under self-recrimination — which means it doesn't get addressed, which means it will surface again.
In therapy, I draw on ACT and self-compassion frameworks to help clients interrupt the shame spiral before it takes hold. We also often work with the inner critic through a parts-based lens — understanding what that critical voice is trying to do, and why — which reduces its grip considerably over time.
And, a clean repair after a blow-up — I snapped, I'm sorry for how it came out, here's what I was actually trying to say — is a skill. And it is absolutely learnable.
What can you actually do when you feel yourself flooding?
Most advice for managing anger focuses on techniques that feel either patronising or impossible once you're already in the heat of it. If you've ever tried to "just breathe" while genuinely flooded, you'll know why that often doesn't work.
What actually interrupts a flooding response has to work with the physiology of the moment. When the nervous system is activated, the most reliable first move is creating a pause before language — not reaching immediately for words. Extended exhales are the most accessible entry point: breathing in for four counts and out for six to eight activates the parasympathetic nervous system within sixty to ninety seconds.
Changing the sensory environment works through a similar mechanism — cold water on the face or wrists, stepping outside, sixty seconds of movement. From a slightly calmer physiological state, a brief verbal signal becomes possible: I'm at capacity. I need ten minutes so I don't say this badly. I'll come back.
That is containment, not avoidance. It protects both the relationship and your dignity within it.
In CBT-informed work, I help clients identify their personal early warning signs — the particular physical or cognitive cues that arrive before full flooding — so the pause can happen earlier, when it's easiest. In ACT, we work on defusion: creating a little distance from the thought or feeling so it stops dictating the next action automatically.
How do you build more emotional buffer between episodes?
Prevention gets a complicated reputation in these conversations because it so easily tips into another performance project — more self-optimization, more things to track, more ways to fall short. That is not what this is about.
What actually builds emotional buffer over time is less about adding practices and more about reducing chronic drain. Sleep is the highest-leverage variable — not perfect sleep, but consistent sleep: a regular wake time, a predictable wind-down, fewer open loops running in the background at night.
Fuel steadiness matters more than most women realize. Protein and fibre earlier in the day, and something substantial during the afternoon window, can significantly reduce reactivity across the whole day. Nervous system recovery — brief, daily, genuinely non-negotiable — looks different for every woman, but small deposits made regularly matter more than occasional large ones.
And alongside all of this: honest attention to the relational and structural factors that are steadily draining the system. If anger keeps returning to the same patterns and contexts, buffer-building alone will not be sufficient. That is a signal worth taking to therapy, not managing around.
In my work with clients, this is where the different modalities I draw on come together — CBT for identifying and shifting the patterns that exhaust you, ACT for clarifying what you actually want to protect, mindfulness for building the moment-to-moment awareness that makes any of it possible to sustain.
📖 Support in perimenopause often looks like less pushing, more steadiness—I unpack that here: How to Support Yourself in Perimenopause (Without Pushing Yourself Harder).
FAQs
Is perimenopause rage a real thing, or am I just stressed? It's real — and it's usually both. Hormonal fluctuations during perimenopause can genuinely lower your frustration threshold and reduce your nervous system's recovery time. But stress, burnout, and accumulated inequity are almost always in the mix too. The question isn't which one is causing it — it's understanding how they're interacting so you can address both.
Why is my anger so much worse some weeks and then fine the next? Hormonal variability — not just decline — is the key driver. Estrogen and progesterone fluctuate unpredictably during perimenopause, affecting the neurotransmitters most closely tied to mood regulation. Your reactivity can spike without any obvious external trigger and shift week to week. Tracking this pattern, ideally with therapeutic support, tends to reduce the disorientation considerably.
Could my rage actually be depression in disguise? It can be, and this is worth taking seriously. Irritability is a commonly underrecognised presentation of depression — particularly in women, who are less likely to present with the "classic" low mood and more likely to present with agitation, frustration, and emotional volatility. If the rage feels more like a constant, grinding edge than spikes with calmer periods in between, that's worth exploring with a professional. The National Institute of Mental Health recognizes irritability as a key symptom of depression — one that's particularly common in women.
How do I stop the shame spiral from making things worse? Recognise that shame is physiologically counterproductive — it tightens the nervous system and increases the likelihood of the next spike. A clean, brief repair is more effective than extensive self-criticism: acknowledge what happened, name what was underneath it, and make one concrete change. In therapy we work on this directly, because the shame response is often one of the most entrenched and most treatable parts of the whole picture.
When should I actually talk to someone about this? Sooner than most women do. If rage is affecting your relationships, your sense of self, or your day-to-day functioning, that's already a meaningful signal — not a threshold you need to cross before you're allowed to ask for support. A GP or menopause specialist can address physical contributors. A therapist can help with regulation, shame, the boundary work, and the bigger identity questions this stage reliably surfaces.
What I want you to hold onto
You are not becoming an angry woman. You are becoming a woman who is harder to take advantage of — harder to convince that what's unfair is fine, harder to persuade that your needs are an inconvenience.
That is uncomfortable. Sometimes for you, and sometimes for the people around you.
But the goal of this work is not to make you easier to be around. It is to help you feel steady enough that your anger becomes useful — something you can hear clearly, act on intentionally, and put down when you're done with it.
Not suppressed. Not weaponized. Yours, and useful.
📖 If you’re building a clearer picture of what’s happening in your midlife body and mind, you can explore the full Definitive Guide to Perimenopause and Mental Health here.
If something in this post resonated with you, I'd love to help you explore it further. I'm Kira Hensley, a Registered Psychotherapist based in Whitby, Ontario, specializing in women's mental health, anxiety, and perimenopause. I offer in-person sessions at my Whitby practice for women in Durham Region, and virtual sessions for women across Ontario.
References
Freeman, E. W., & Sammel, M. D. (2016). Anxiety as a risk factor and outcome associated with menopausal hot flashes. Menopause, 23(10), 1156–1162.
Bromberger, J. T., & Kravitz, H. M. (2011). Mood and menopause: Findings from the Study of Women's Health Across the Nation (SWAN) over ten years. Obstetrics and Gynecology Clinics of North America, 38(3), 609–625.
The Menopause Society. (2023). Menopause and mental health.
The information on this website is for informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment or to replace your relationship with your health care provider. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read or seen on this site.